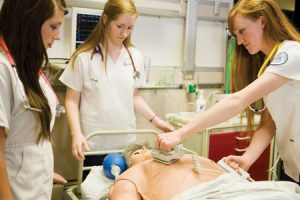
Most patiently, Sam awaits his fate at the hands of (left to right) Rachel Herrmann Lark (’12), Amy Madsen Hermann (’11), and Kirtley A. Sorensen (’10).
Reggie’s tattooed arm lies motionless on the hospital bed as four nurses count CPR cycles. The epinephrine isn’t working. Neither is the defibrillator. “What’s going on?” asks the doctor, arriving on scene.
“He’s, um, bleeding from the stomach. We took out 600 CCs of blood.”
“How long has CPR been going?”
“About 20 minutes, and we shocked him twice.”
“Let’s call it.”
It takes a second for the shock to register on everyone’s faces.
Reggie is dead.
“Oh my gosh! That’s depressing,” says one student nurse. Another throws her notebook onto the nearby crash cart. The rest dissolve into laughter, dispelling the tension.
And laughing is OK—Reggie is a mannequin.
The “doctor,” played by University Hospital ICU nurse Shawn Theobald, a teaching assistant at BYU, preps students for the next scenario with the $80,000 high-fidelity “Sam” mannequin. Sam, as the students named him, takes on many different personas—like Reggie—for the scenarios. Sam’s green tattoos can be swapped for black ones; his wigs include business cuts, dreadlocks, and longer locks for when he becomes a she. And Sam is a sophisticated guy. He breathes and bleeds and responds to treatment as though he were a real patient.
BYU has four high-fidelity and 12 mid-fidelity mannequin patients living in hospital beds in BYU’s Nursing Learning Center (NLC), a somewhat cramped facility in the basement of the SWKT. Thanks to a recent $4 million grant from the Fritz B. Burns Foundation, the college plans to remodel the facility in 2013. The expansion will improve the hands-on mannequin labs, which are part of a growing trend in nursing education—a trend BYU helped set.
“We were at the forefront of moving with [the simulations],” explains associate dean Patricia K. Ravert (BS ’75), who incorporated the first $250,000 Sam mannequin into BYU’s curriculum in 2001. As the research advisor for the International Nursing Association for Clinical Simulation and Learning, Ravert is immersed in the application of simulation in nursing education, which allows students to practice skills in a safe but realistic environment. Saving Sam and other mannequins in distress “gives [students] the opportunity to learn to prioritize, delegate, critically think, and figure out things together,” says Ravert.
In a single semester at BYU, Sam undergoes 160 different scenarios, rotating through 64 students for each one. He dies in around 14 of those scenarios and experiences cardiac arrest in 60, in addition to experiencing respiratory arrests, gastrointestinal bleeds, diabetic comas, and other common ailments. Just like a real patient, Sam’s baby blues both blink and dilate and he breathes with a rising and falling chest. His heart produces various programmable rhythms detectable from his carotid artery to his feet. Hurt him too much and he’ll start to cry from his functional tear ducts. Most important, mistakes can be fatal. Luckily, he comes back to life.
Meet Sam’s Fam
Giving birth every 20 minutes, Noelle can get a bit feisty, with pre-programmed phrases such as “Ouch,” “Don’t touch me,” and “This is all your fault.” With an internal hydraulic system, she delivers a mannequin baby—unless there’s a breach delivery or C-section.
This cutie is everyone’s favorite. “It’s like playing dolls on steroids,” says Colleen R. Tingey (BS ’88), Nursing Learning Center supervisor. “[Hal] has arms that move, and he cries and his cheeks turn blue.” He feels like a real baby and even has an umbilical chord with a pulse that can receive IVs.
Samantha, the pediatric mannequin, is somewhat “facially challenged,” says visiting professor Debra K. Wing (’82). “She always looks, bless her heart, like she got caught in a wind tunnel.” To help, they’ve given her earrings and a hat. Samantha goes through a severe asthma attack about six times a semester and gets an endotracheal tube placed in her throat.
Practicing on Sam is about as close to real life as it gets with a plastic patient. Operated by a computer, he automatically responds to drugs, “speaks” through an instructor microphone, responds to electric shock in defibrillation, and even becomes a woman when necessary.
One of the college’s 12 less-sophisticated VitalSim models, this $6,800 mannequin takes some of the pressure off Sam’s job by providing opportunities for students to practice basic skills such as the checking of vital signs; listening to heart, bowel, and lung sounds; and practicing IVs, bed baths, and more.